Big Toe Pain May Mean Gout
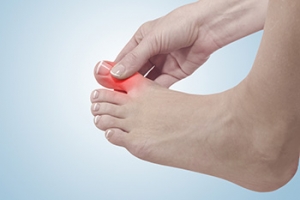
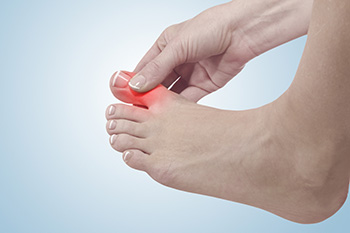 Gout, a type of arthritis, can cause intense pain that often starts in the big toe. This condition is caused by a build up of needle shaped uric acid crystals in the joints, leading to inflammation. The big toe is where painful gout attacks commonly occur because it is a cooler part of the body, and uric acid is more likely to crystallize there. Gout patients usually experience painful joint flares for a week or so, which then disappear for a period of time. Some patients do not experience their next flare for a year or more. Lifestyle factors such as a diet particularly rich in purine-containing foods in addition to genetics can contribute to gout development. During a gout flare up, the big toe may become red, swollen, and extremely tender. It is essential for those experiencing big toe pain to seek medical attention, as managing gout requires having a well informed plan. If you have pain in your big toe and suspect it may be gout, it is suggested you schedule an appointment with a podiatrist who can help you find relief from the acute pain associated with this condition.
Gout, a type of arthritis, can cause intense pain that often starts in the big toe. This condition is caused by a build up of needle shaped uric acid crystals in the joints, leading to inflammation. The big toe is where painful gout attacks commonly occur because it is a cooler part of the body, and uric acid is more likely to crystallize there. Gout patients usually experience painful joint flares for a week or so, which then disappear for a period of time. Some patients do not experience their next flare for a year or more. Lifestyle factors such as a diet particularly rich in purine-containing foods in addition to genetics can contribute to gout development. During a gout flare up, the big toe may become red, swollen, and extremely tender. It is essential for those experiencing big toe pain to seek medical attention, as managing gout requires having a well informed plan. If you have pain in your big toe and suspect it may be gout, it is suggested you schedule an appointment with a podiatrist who can help you find relief from the acute pain associated with this condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Anas Khoury, DPM from North Eastern Foot & Ankle Specialists. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Passaic, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Gout
Gout is a form of arthritis that is caused by a buildup of uric acid crystals in the joints. This considered to be one of the most frequently recorded medical illnesses throughout history. Gout occurrences in the US have risen within the past twenty years and the condition now affects 8.3 million people which is 4% of all Americans. Researchers have found that gout affects men more than women and African-American men more than white men.
Symptoms of gout are warmth, swelling, discoloration, and tenderness in the affected joint area. The small joint on the big toe is the most common place for a gout attack to occur.
People who are obese, gain weight excessively, drink alcohol heavily, have high blood pressure, or have abnormal kidney function are more likely to develop gout. Furthermore, certain drugs and diseases are likely to increase levels of uric acid in the joints which eventually leads to gout. You are also more likely to develop gout if you eat a lot of meat and fish.
Many who experience gout attacks will experience repeated attacks over the years. Some people who have gout symptoms, may never have them again, but others may experience them several times a year. If you have gout symptoms throughout the year, you may have recurrent gout. Those who have gout should also be careful about their urate crystals collecting in their urinary tract, because this may lead to kidney stones.
Diagnosis for gout is done by checking the level of uric acid in the joints and blood. Your podiatrist may also prescribe medicine to reduce uric acid buildup in the blood, which will help prevent any gout attacks.
To treat gout, your podiatrist may also prescribe you Anti-inflammatory medication (NSAIDs) which will relieve the pain and swelling of a gout episode and it can also shorten a gout attack. Maintaining a healthy diet is also a proven method to prevent gout attacks.
Choosing the Right Ankle Brace
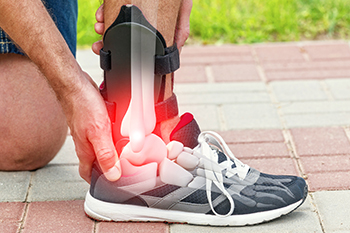
Selecting the appropriate ankle brace is akin to navigating a complex landscape, especially given the diverse needs of athletes. Ankle injuries demand tailored solutions, and understanding the attributes of each brace type is important. Sleeves, while the least stable, offer comfort and are suitable for first-line treatment. Straps, popular among athletes, involve cloth straps that create a heel-lock figure-eight, yet their complexity can lead to adherence issues. Stirrups, popular in the 90s, now find use in splints and controlled ankle motion. Lace-ups, the original stable design, have evolved with improvements in functionality and comfort. Hybrid braces, combining features of sleeves, straps, stirrups, and lace-ups, offer both comfort and stability, but come at a higher cost. The choice among these types depends on factors such as the athlete's position, preferences, and the specific injury or condition being addressed. It is suggested that you schedule an appointment with a podiatrist to find the most suitable brace for you.
Ankle and foot injuries are common among athletes and in many sports. They can be caused by several problems and may be potentially serious. If you are feeling pain or think you were injured in a sporting event or when exercising, consult with Anas Khoury, DPM from North Eastern Foot & Ankle Specialists. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Common Injuries
The most common injuries that occur in sporting activities include:
- Achilles Tendonitis
- Achilles Tendon Rupture
- Ankle Sprains
- Broken Foot
- Plantar Fasciitis
- Stress Fractures
- Turf Toe
Symptoms
Symptoms vary depending upon the injury and in some cases, there may be no symptoms at all. However, in most cases, some form of symptom is experienced. Pain, aching, burning, bruising, tenderness, tightness or stiffness, sensation loss, difficulty moving, and swelling are the most common symptoms.
Treatment
Just as symptoms vary depending upon the injury, so do treatment options. A common treatment method is known as the RICE method. This method involves rest, applying ice, compression and elevating the afflicted foot or ankle. If the injury appears to be more serious, surgery might be required, such as arthroscopic or reconstructive surgery. Lastly, rehabilitation or therapy might be needed to gain full functionality in the afflicted area. Any discomfort experienced by an athlete must be evaluated by a licensed, reputable medical professional.
If you have any questions, please feel free to contact our office located in Passaic, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are common among athletes and those who exercise frequently. Most of these injuries are non-life-threatening and can heal in weeks with proper treatment and care. Serious injuries, however, require urgent medical treatment.
Common minor injuries include ankle sprains, ankle strains, Achilles tendonitis, plantar fasciitis, stress fractures, and turf toe. An ankle sprain is when the ligaments in the ankle have either become stretched or torn. When the muscle or tendon is stretched or torn, it is an ankle strain. When the big toe is sprained, it is known as turf toe. Achilles tendonitis is the overuse and inflammation of the Achilles tendon. Plantar fasciitis is the inflammation of the plantar fascia and generally occurs from overuse in athletics. Stress fractures are also caused from overuse and are small cracks in the bone.
Achilles tendon ruptures are common, but more serious. This injury occurs when the Achilles tendon, the largest tendon in the body, ruptures. In most cases, this causes severe pain and difficulty walking; some who have experienced this injury have reported, however, no signs or symptoms. A laceration is a deep cut that can occur anywhere on the body. Lacerations on the foot are rarer, but can occur from things like metal cleats landing on the foot.
Treatment options cover a wide range of methods based upon the injury and its severity. Conditions like plantar fasciitis, stress fractures, Achilles tendonitis, turf toe and ankle sprains/ strains can heal on their own without immediate medical care, but seeing a podiatrist to monitor the injury is always recommended. Following the RICE (Rest, Icing, Compression, and Elevation) protocol is generally enough to treat minor injuries. This means resting the foot by either keeping pressure off the foot or not walking at all. Icing the injury will help reduce swelling and pain. Compressing the wound with a wrap will immobilize and help promote healing. Finally, keeping the wound elevated will also reduce swelling and also help the healing process.
It is important to note that even minor injuries can vary in severity, with grade one being a minor injury and grade three requiring urgent care by a podiatrist. Achilles tendon ruptures and lacerations on the foot generally require urgent medical care and treatment options that need a podiatrist. These could include imaging tests, stitches for cuts, rehabilitation, and casts or braces. Every case is different, however, so it is always recommended to see a podiatrist when pain in the foot does not disappear.
See Your Foot Specialist Regularly If You Work On Your Feet
Progression of Diabetic Foot Problems
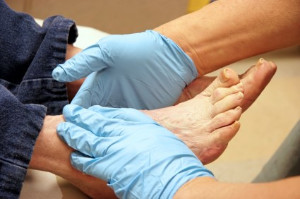
Diabetic foot problems associated with diabetes mellitus can affect one or both feet in type one or type two diabetes cases. These issues, often linked to nerve damage and circulatory problems inherent to diabetes, exhibit symptoms over time. Common diabetic foot problems include skin complications and structural foot alterations, foot ulcers, infections, and foot structure changes. The root cause of diabetic foot problems lies in inadequate insulin regulation, as diabetes disrupts insulin production or responsiveness. Elevated blood sugar levels, over time, inflict nerve damage, leading to peripheral neuropathy and hindered blood circulation, resulting in peripheral artery disease, or PAD. Peripheral neuropathy symptoms can consist of numbness, tingling, and diminished sensation in the feet, making ulcer detection challenging. Left untreated, infections can fester due to impaired blood flow, potentially leading to gangrene and tissue death. Early-stage diabetic foot problems often go unnoticed but can be identified by leg pain, numbness, and skin changes. Timely intervention is crucial. Diabetic foot issues progress at varying rates. Untreated complications may entail ulcers, corns, deformities, muscle weakness, and impaired blood flow. Seeking professional treatment for wounds and infections is vital, with treatments like wound dressings, antibiotics, off-loading devices, and debridement. In severe cases, surgical intervention, such as vascular procedures, skin grafts, or deformity correction may be necessary. If you suffer from diabetic foot problems, it is strongly suggested that you schedule regular appointments with a podiatrist to monitor your feet and do all that is necessary to prevent problems from arising and taking care of those that do.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Anas Khoury, DPM from North Eastern Foot & Ankle Specialists. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Passaic, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Care
Diabetes can cause two problems that can potentially affect the feet: Diabetic neuropathy and Peripheral Vascular Disease. Diabetic neuropathy occurs when nerves in your legs and feet become damaged, which prevents you from feeling heat, cold, or pain. The problem with diabetic neuropathy is that a cut or sore on the foot may go unnoticed and the cut may eventually become infected. This condition is also a main cause of foot ulcers. Additionally, Peripheral vascular disease also affects blood flow in the body. Poor blood flow will cause sores and cuts to take longer to heal. Infections that don’t heal do to poor blood flow can potentially cause ulcers or gangrene.
There are certain foot problems that are more commonly found in people with diabetes such as Athlete’s foot, calluses, corns, blisters, bunions, foot ulcers, ingrown toenails, and plantar warts. These conditions can lead to infection and serious complications such as amputation. Fortunately, proper foot care can help prevent these foot problems before they progress into more serious complications.
Each day you should wash your feet in warm water with a mild soap. When you finish washing your feet, dry them carefully especially between your toes. You should also perform daily foot inspections to ensure you don’t have any redness, blisters, or calluses. Furthermore, if you are diabetic, you should always wear closed-toed shoes or slippers to protect your feet. Practicing these tips will help ensure that your feet are kept healthy and away from infection.
If you have diabetes, contact your podiatrist if you have any of the following symptoms on your feet: changes in skin color, corns or calluses, open sores that are slow to heal, unusual and persistent odor, or changes in skin temperature. Your podiatrist will do a thorough examination of your feet to help treat these problematic conditions.
Triggers of Plantar Warts
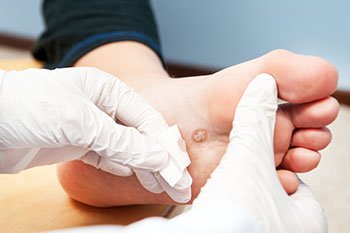
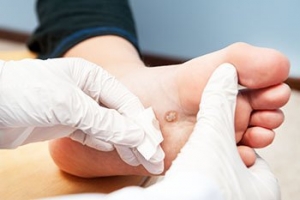
Plantar warts, small growths caused by the human papillomavirus, or HPV, are notorious for cropping up on the soles of the feet, bringing discomfort and annoyance. Understanding the triggers behind their occurrence is essential for prevention. The virus thrives in warm, moist environments, making communal spaces like swimming pools, locker rooms, and public showers prime breeding grounds. Walking barefoot in these areas increases the risk of viral exposure. Additionally, cuts or abrasions on the soles create entry points for the virus, facilitating infection. Weakened immune systems, often seen in individuals under stress or with underlying health conditions, make them more susceptible to plantar warts. While direct contact with the virus is the primary mode of transmission, the virus can also be contracted indirectly through contaminated surfaces. Awareness of these triggers empowers individuals to adopt preventive measures, such as wearing protective footwear in public areas and maintaining foot hygiene, to thwart the onset of plantar warts. If you have developed a plantar wart, it is suggested that you consult a podiatrist who can offer the treatment method that is best for you.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Anas Khoury, DPM from North Eastern Foot & Ankle Specialists. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Passaic, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Warts
Plantar warts are growths that typically appear on the heels or other weight-bearing areas of the feet. These warts are caused by the human papillomavirus (HPV). The virus enters the body through breaks in the skin, such as cuts, that are on the bottom of the feet. Plantar warts are more likely to affect children and teenagers, people with weakened immune systems, people who have a history with plantar warts, and people who walk barefoot in environments exposed to a wart-causing virus.
If you suspect you have plantar warts, you may have the following symptoms: pain or tenderness while walking, a lesion that interrupts the ridges in the skin of your foot, small fleshy lesions on the bottom of the foot, or a callus where a wart has grown inward over a well-defined spot on the skin.
HPV causes plantar warts to form and is very common. There are more than 100 kinds of the virus in existence. However, only a few of them cause warts on the feet. The other types of HPV are likely to cause warts on other parts of the body.
If you have plantar warts, your podiatrist may try different treatment methods depending on your specific case. Some treatments for plantar warts are peeling medicines (salicylic acid), freezing medicines (cryotherapy), or surgical procedures. Laser treatments and vaccines are also used to treat plantar warts.
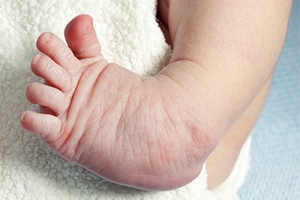
Clubfoot Is a Congenital Foot Condition
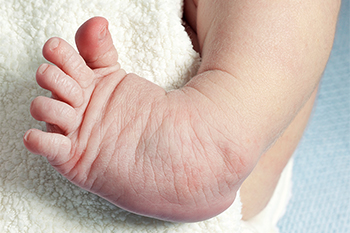
Clubfoot, a congenital condition affecting newborns, is characterized by the abnormal positioning of the foot or feet. This condition is present at birth, with the infant's foot turning inward and downward, resembling the club's head. The primary causes of clubfoot are often linked to a combination of genetic and environmental factors. While the exact genetic mechanisms are not fully understood, there is evidence of familial predisposition. Environmental factors, such as intrauterine positioning or limited space in the womb, can also contribute to the development of clubfoot. This congenital anomaly affects the muscles, tendons, and bones in the foot, leading to a tightened Achilles tendon and an imbalance in the surrounding structures. Early detection and intervention are crucial for managing clubfoot effectively. Treatment options may include gentle stretching, casting, and, in some cases, surgical procedures to correct the foot's alignment and promote proper development. If your child has been born with clubfoot, it is strongly suggested that a podiatrist is on your healthcare team who can determine what the best treatment option is for this condition.
Congenital foot problems require immediate attention to avoid future complications. If you have any concerns, contact Anas Khoury, DPM of North Eastern Foot & Ankle Specialists. Our doctor can provide the care you need to keep you pain-free and on your feet.
Congenital foot problems are deformities affecting the feet, toes, and/or ankles that children are born with. Some of these conditions have a genetic cause while others just happen. Some specific foot ailments that children may be born with include clubfeet, polydactyly/macrodactyly, and cleft foot. There are several other foot anomalies that can occur congenitally. What all of these conditions have in common is that a child may experience difficulty walking or performing everyday activities, as well as trouble finding footwear that fits their foot deformity. Some of these conditions are more serious than others. Consulting with a podiatrist as early as possible will help in properly diagnosing a child’s foot condition while getting the necessary treatment underway.
What are Causes of Congenital Foot Problem?
A congenital foot problem is one that happens to a child at birth. These conditions can be caused by a genetic predisposition, developmental or positional abnormalities during gestation, or with no known cause.
What are Symptoms of Congenital Foot Problems?
Symptoms vary by the congenital condition. Symptoms may consist of the following:
- Clubfoot, where tendons are shortened, bones are shaped differently, and the Achilles tendon is tight, causing the foot to point in and down. It is also possible for the soles of the feet to face each other.
- Polydactyly, which usually consists of a nubbin or small lump of tissue without a bone, a toe that is partially formed but has no joints, or an extra toe.
- Vertical talus, where the talus bone forms in the wrong position causing other bones in the foot to line up improperly, the front of the foot to point up, and the bottom of the foot to stiffen, with no arch, and to curve out.
- Tarsal coalition, when there is an abnormal connection of two or more bones in the foot leading to severe, rigid flatfoot.
- Cleft foot, where there are missing toes, a V-shaped cleft, and other anatomical differences.
- Macrodactyly, when the toes are abnormally large due to overgrowth of the underlying bone or soft tissue.
Treatment and Prevention
While there is nothing one can do to prevent congenital foot problems, raising awareness and receiving neonatal screenings are important. Early detection by taking your child to a podiatrist leads to the best outcome possible.
If you have any questions please feel free to contact our office located in Passaic, NJ . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.